
What Is Peripheral Neuropathy?
Peripheral neuropathy is a disorder involving damage to the peripheral nerves outside the brain and spinal cord, causing disruptions in sensation, muscle control, and organ function. These nerves are responsible for sending sensory information to the central nervous system and relaying commands from the brain and spinal cord to the rest of the body. When damaged, the communication between your body and brain gets interrupted, resulting in various symptoms.
Peripheral neuropathy is surprisingly common, affecting millions globally with issues ranging from mild numbness to severe motor difficulties. Symptoms tend to develop gradually and worsen over time if left unmanaged. Early understanding and proactive management are essential to curb its progression and improve daily life, making education an important first step for anyone facing this diagnosis.
Many people seek out Peripheral Neuropathy Treatment when typical symptoms like tingling, burning pain, or weakness begin to interfere with activities or sleep. These symptoms often start subtly and may at first be dismissed as a regular part of aging, but they can quickly escalate if not addressed. Timely intervention can mitigate symptom escalation, minimize long-term damage, and enhance quality of life by addressing the condition’s cause and daily impact. Consulting a healthcare professional as soon as symptoms arise can lead you to successful management.
Common Symptoms and Causes
The sensory changes induced by peripheral neuropathy are often described as “pins and needles,” numbness, burning, and pain—particularly in the hands and feet. Some people also report sensations of buzzing, sharp jabs, or hypersensitivity to touch, making simple tasks like walking or buttoning a shirt challenging. Additional warning signs might include loss of coordination, muscle weakness, or balance issues, increasing the risk of falls and making daily activities more difficult. In severe cases, changes to autonomic functions—like digestion, heart rate, or sweating—may occur, compounding the effect on overall health.
These symptoms can stem from diverse causes, including diabetes (the leading cause), autoimmune disorders such as lupus or rheumatoid arthritis, certain viral or bacterial infections, vitamin deficiencies—especially B vitamins, and traumatic injuries. Some chemotherapy drugs and other medications can also have neurotoxic effects, leading to neuropathy.
Early recognition is key. If you notice abnormal sensations, muscle weakness, or trouble with coordination, consult your healthcare provider promptly for a complete neurological evaluation. An accurate diagnosis is critical for identifying the underlying cause, tailoring treatment, and making lifestyle adjustments to prevent further nerve deterioration.
Daily Adjustments for Better Comfort
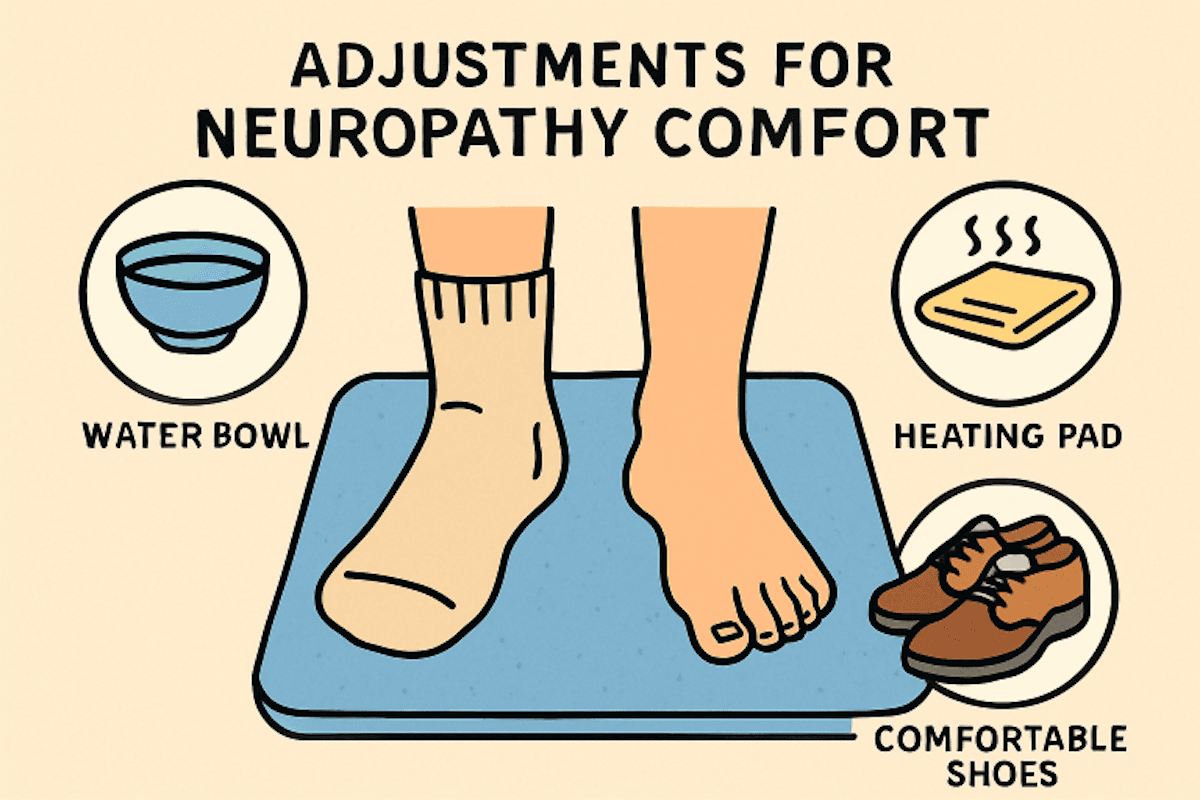
Small lifestyle shifts can meaningfully reduce everyday discomfort associated with peripheral neuropathy. Simple measures such as warm foot soaks can increase blood flow and soothe aches, while wearing comfortable, cushioned socks helps reduce friction that could injure sensitive skin. Placing nonslip mats in high-traffic areas and ensuring floors are free of obstacles can help safeguard sensitive feet and prevent falls—a common concern when numbness or balance issues are present.
For those who experience heightened temperature sensitivity, tools such as heated blankets, thermal gloves, or cooling pads can reduce symptom flare-ups and help maintain comfort in changing environments. Gentle stretching and movement practices like chair yoga improve flexibility and support circulation, which is beneficial for nerve health. Regular periods of rest throughout the day can help manage fatigue, giving your nerves a chance to recover and reducing the impact of overexertion.
Lifestyle Tips That Slow Progression
- Keep blood sugar levels within healthy ranges to prevent diabetic neuropathy. If you have diabetes, consistent glucose monitoring and adherence to your prescribed diet and medication plan can make a significant difference in stabilization and even symptom improvement.
- Choose a balanced diet featuring B vitamins, vitamin E, whole grains, fruits, and vegetables, all of which are crucial for nerve health. Ensuring adequate nutrition helps the body repair itself and may slow disease progression.
- Limit alcohol consumption, as it can contribute to nerve degeneration. Even moderate levels of alcohol can worsen symptoms or interact negatively with medications prescribed for neuropathy.
- Stop smoking to enhance blood flow and healing throughout the nervous system. Smoking reduces circulation, which increases the risk of further nerve damage and slows the body’s healing processes.
Make regular check-ups and bloodwork part of your routine, particularly if you have underlying health conditions. This proactive approach allows for early detection of any new complications and provides the opportunity for timely adjustments to your treatment plan. Adequate sleep gives your body time to heal, while removing unnecessary stressors and practicing mindfulness or relaxation techniques can also strengthen your body’s resilience against neuropathy progression.
Treatment Options and Support
Peripheral neuropathy can be managed using a blend of medications, self-care, and rehabilitation approaches. Over-the-counter pain relievers, topical creams containing CBD, capsaicin, menthol, or lidocaine, and prescription medications like anticonvulsants or antidepressants often offer significant symptom relief. If pain remains severe, your healthcare provider might suggest alternative interventions such as nerve blocks or transcutaneous electrical nerve stimulation (TENS).
In persistent cases, physical or occupational therapy is valuable in providing strategies for protecting affected limbs, optimizing mobility, reducing fall risk, and maintaining independence. Custom orthotics or splints may be prescribed to provide extra support and alleviate mechanical stress on joints and nerves. According to the National Institute of Neurological Disorders and Stroke, new research into nerve regeneration and electrical nerve stimulation is quickly gaining momentum, offering hope for those living with chronic symptoms and fostering optimism for the future.
Staying Active Safely
Physical activity is essential, but it’s best approached with caution when dealing with peripheral neuropathy. Low-impact exercises like walking, swimming, or stationary cycling can improve circulation and maintain muscle strength without overtaxing vulnerable nerves. Stretching routines, tai chi, or light resistance training provide further opportunities to support physical function without excessive risk.
Set realistic movement goals that honor individual limits, and always wear supportive, protective footwear and use assistive devices as your healthcare provider recommends. To prevent injury, ensure thorough warm-ups and cool-downs with each exercise session, and pay attention to your body’s cues to avoid overexertion or strain.
Mental Health and Support Networks
Chronic symptoms often carry an emotional burden, manifesting as frustration, stress, or feelings of isolation. According to Mayo Clinic resources, emotional health is essential in symptom management and promoting resilience during challenging times. The unpredictability of neuropathic pain and loss of mobility can contribute to mood swings and decreased self-esteem, making emotional support just as important as physical care.
Building a strong support network is vital to emotional well-being. Engage in local or virtual support groups, talk openly with friends and family, and consider speaking with a counselor or therapist who has experience with chronic illness. Incorporate mindfulness meditation, guided relaxation, or deep-breathing exercises into your daily routine to lower anxiety and improve overall mood.
Innovations in Peripheral Neuropathy Research
Advancements in neurology are increasingly hopeful, with research focusing on early diagnostic tools, new pharmacological approaches, and regenerative medicine. Scientists are now exploring stem cell therapies, gene therapies, and novel biologics that offer the potential to directly repair or regenerate damaged nerves rather than only manage symptoms. Improvements in noninvasive imaging and wearable monitoring technology are making diagnosis and individualized treatment more accessible.
Staying informed about ongoing research can empower individuals with peripheral neuropathy to explore new options as they become available. Following updates from leading neurological organizations keeps you at the forefront of these developments—because as treatment options expand, so does the potential for a more comfortable, active life. Hope remains strong that the future will offer not just better management of peripheral neuropathy, but the possibility of meaningful recovery.
For more information on recent research, visit the Foundation for Peripheral Neuropathy Research.
Pin This Post




